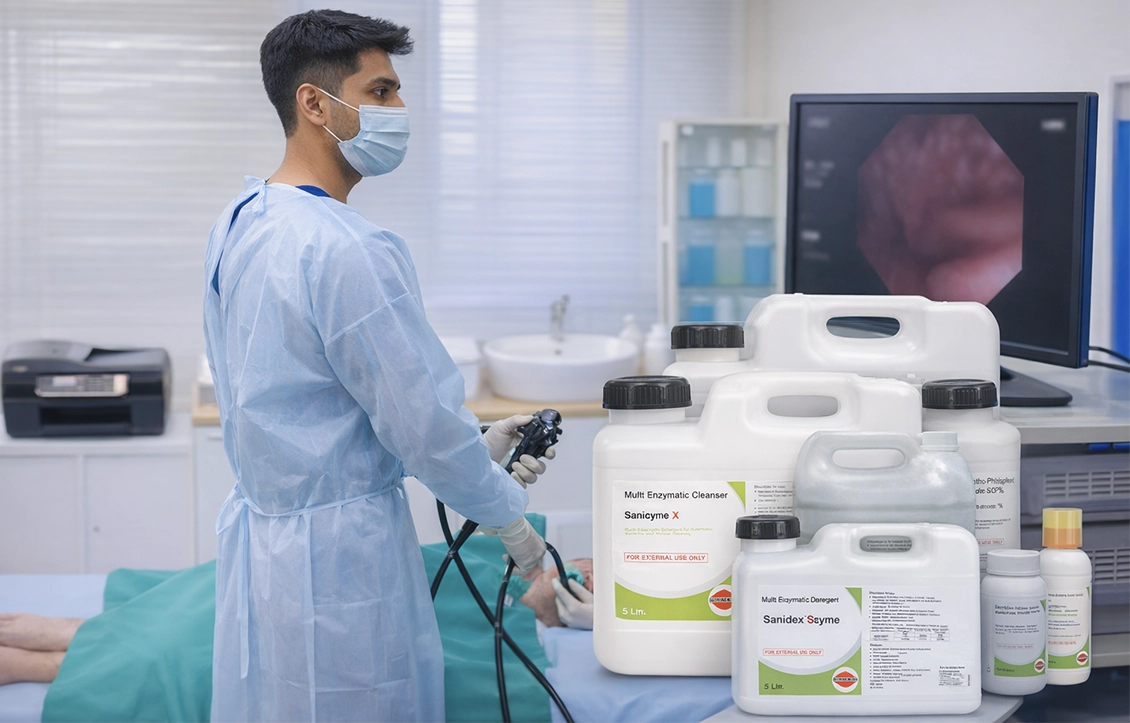
An endoscopy is a vital diagnostic and therapeutic minimally invasive medical procedure where a doctor inserts a thin, flexible tube (endoscope) via the mouth, anus, or a small incision to examine areas such as the esophagus, stomach, colon, or lungs.
Most endoscopes have a light and a specialized camera at the end. The scope captures images or videos of organs or other body parts and displays them on a screen that a healthcare professional can see. Doctors use them to treat diseases of the internal organs without major surgery.
Despite its clinical advantages, the procedure carries low infection risks that demand attention from hospitals seeking to optimize patient safety and operational efficiency. Understanding endoscopy infection risk is imperative for implementing effective mitigation strategies and strengthening infection prevention protocols.
Types of Endoscopy Infection Risk & Prevalence
Endoscopy procedures carry low but notable risks of infection, mainly because of inadequate reprocessing of endoscopes, leading to both endogenous and exogenous transmissions.
Endoscopic infections generally fall into 2 categories:
1. Exogenous Infections (Transmission via Equipment)
Exogenous infections happen via transmission through inadequately reprocessed endoscopes, accessories (e.g., biopsy forceps), or staff contact, often involving resilient pathogens.
Here are the common culprits: Pseudomonas aeruginosa (biofilm-forming, frequent in ERCP outbreaks), non-tuberculous mycobacteria, Salmonella spp. (GI scopes), and multidrug-resistant Klebsiella or E. coli.
2. Endogenous Infections (Patient’s Own Flora)
Endogenous infections occur from translocation of the patient’s normal flora during mucosal disruption; they are more common overall but difficult to prevent via equipment alone.
Here are the common culprits: E. coli, Klebsiella spp., Enterobacter spp., enterococci; higher in biliary stenting.
Prevalence
Contamination rates of endoscopes range from 7.7% to 34.6%, based on the type of device utilized. Duodenoscopes, whether used for ERCP (Endoscopic Retrograde Cholangiopancreatography) or EUS (Endoscopic Ultrasound), have reported contamination rates between 0.697% and 60%.
Key Factors Influencing Risk
Risk factors associated with post-endoscopic infections include:
1. Reprocessing Failures
Improper cleaning, biofilms, or damaged or complex equipment design.
2. Insufficient Drying or Storage
Failure to properly dry channels with 70% alcohol and forced air makes a suitable environment for the bacteria to grow during storage.
3. Patient Individual Factors
Age above 65, male, immunosuppression, cirrhosis (viral/alcoholic), CKD, cholangiocarcinoma, chemotherapy.
4. Complexity of the Procedure
Therapeutic interventions such as stenting and dilation have a higher risk than diagnostic ones.
5. Biofilm Formation
Microorganisms form biofilms on the endoscope or within automated endoscope reprocessors (AERs).
What Hospitals and Staff Must Do to Minimize the Risk
Hospitals and staff play a vital role in minimizing endoscopy infection risks via standardized protocols and vigilant execution.
1. The Chain of Infection Control
Endoscopes are categorized as semi-critical medical devices, meaning they must be cleaned using high-level disinfection.
Hence, block pathogen transmission by following these seven steps: (1) Pre-cleaning, (2) Leak testing, (3) Manual cleaning (brushing or flushing), (4) Visual inspection, (5) High-Level Disinfection (HLD), (6) Drying or storage, and (7) Documentation.
2. Combat Biofilm Formation (Sticky Microbial Communities in Endoscope Channels)
Disrupt the biofilm formation by immediately precleaning with enzymatic detergents (Sanizyme manufactured by Sirmaxo), followed by mechanical brushing of all channels.
3. Drying is Mandatory
Wet scopes encourage bacterial growth (up to 1,000-fold in hours); hence, forced-air dry scopes post-alcohol flush and store in ventilated cabinets to maintain dryness and avoid endoscope recontamination.
4. Routine Culturing
Routine microbiological surveillance of reprocessed endoscopes should be done to verify the effectiveness of the disinfection process.
5. Single-Use Adoption
Many hospitals are adopting single-use disposable endoscopes for high-risk procedures, significantly reducing reprocessing failures.
What a Patient Should Do Before & After an Endoscopy Procedure
Here is the quick tip for a patient undergoing an endoscopy procedure
Before Procedure
You can ask this question of the hospital injury team:
- What is your facility’s infection rate for this procedure?
Does the facility follow the ASGE (American Society for Gastrointestinal Endoscopy) guidelines for endoscope reprocessing?
How often does the audit team perform microbiological surveillance on your scopes?
After Procedure
Following an endoscopy, an individual should look for fever, severe or constant abdominal pain, chest pain, shortness of breath, bloody or black stool, or severe sore throat. If the patient notices these signs, they should immediately contact their doctor.
Conclusion
Endoscopy infection risk is measurable and preventable in many cases. For the hospitals and healthcare systems, it’s mandatory to strengthen protocols, improve environmental hygiene, and treat infection prevention as a fundamental operational priority, not an afterthought.
Hospitals seeking top-quality enzymatic detergents for optimal instrument reprocessing can trust Sirmaxo for proven performance and reliability.
Contact Sirmaxo today to elevate your endoscopy protocols
- +91 22 42500800
- +91 22 42500852
- info@sirmaxochem.in
Our Address: 5th Floor, Satyanarayan Prasad Commercial Center, Dayaldas Lane, Off. Nehru Road, Vile Parle (E), Mumbai 400057, India
Our manufacturing units are located at the following locations:
Plot NO:E-35 MIDC-Tarapur, Boisar, Palghar Dist, Maharashtra-401506 India
Plot NO:E-130 & E-130/1, MIDC-Tarapur, Boisar,Palghar Dist, Maharashtra-401506 India